

Several different types of pain blocks are available at our Phoenix pain management clinic; how can you tell them apart? Facet pain blocks and medial branch pain blocks are two of the most common. A facet pain block is a spinal joint injection of anesthetic and steroids. A medial branch pain block is similar to a lateral branch pain block, except that the medication is injected outside the joint and closer to the nerves (the medial branch nerves). A steroid may or may not be used in medial branch pain blocks.
These pain blocks are frequently used in patients who suffer from back pain, which is frequently caused by arthritis and/or mechanical lower back pain. Multiple injections may be necessary depending on the number of affected joints. Additionally, pain blocks can be diagnostic, therapeutic, or a combination of the two. These techniques can be used as diagnostic tools, as a pain block can indicate to a pain specialist whether the pain is coming from a pain-blocked facet joint. In other words, if the pain persists after the pain block is placed, the facet joint is ruled out as a possible source.
Pain management is a branch of medical practice that touts the reduction of pain. Pain management covers a wide range of conditions, including neuropathic pain, sciatica, postoperative pain, and more. Pain management is a burgeoning medical specialty that utilizes a multi-disciplinary approach to treating all kinds of pain. Pain management doctors treat people in pain by evaluating a patient to determine which pain treatment protocol would be best before prescribing rehabilitation protocols. Since pain management doctors utilize a multi-disciplinary model, they typically refer to Doctors of Chiropractic for spinal and manual adjustments or to a Physical therapist for rehabilitative exercises. Your general medical doctor may refer you to pain management when your pain is significant and ongoing.
Medical physicians who specialize in pain management understand the complexities of pain, and a pain physician approaches the problem holistically. While treatment at a pain clinic should ideally be patient-centered, this may not always be the case due to the clinics’ limited resources. There are currently no established standards for the types of disciplines that must be included, which is another reason why treatment options vary between clinics. This article hopes to explain the difference between the Medial Branch Block Vs Facet Joint Injection.
While some types of pain can be chronic, such as headaches and others acute, we focus on auto accident injuries. Our pain management protocols specifically address the root underlying cause of your pain. This allows for the application of science and the latest advances in medicine to relieve your pain. “we now have many modalities, including medication, interventional pain management techniques, nerve blocks, Facet blocks, Trigger point injections, along with Chiropractic Care and management to help reduce your pain. The goal of pain management is to minimize pain rather than eliminate it. Integrating pain management with chiropractic adjustments provides a potent one-two punch at correcting your pain’s underlying root cause of your pain. This is because quite often, it is not possible to do away with it completely. Two other goals are to improve function and increase the quality of life. These three goals go hand-in-hand.
Look for a clinic with a specialist who knows about your kind of pain. Ask if the doctor has had special training and is board certified in pain management. As with other doctors, you should also try to find someone you feel comfortable with. Your pain management specialist will treat your pain and coordinate other care, including physical therapy, rehabilitation, and counseling. A good pain program will work with you and your family to create a plan based on your goals. It will monitor your progress and tell you how you’re doing.
Auto accidents can result in various symptoms throughout the body, depending on the mechanism of injury. Neck, mid-back and lower back pain are all common symptoms, with or without radiating symptoms down the arms and legs. After an auto accident, an initial exam is highly recommended to assess each part of the body and prevent permanent damage to the spine and nerves. Early intervention, such as epidural steroid injections or medial branch blocks, can help prevent pain from becoming chronic, thereby avoiding the need for future invasive surgeries and procedures. At Phoenix Pain Treatment Clinic in West Phoenix, Arizona, our pain specialists conduct thorough examinations and utilize state-of-the-art diagnostic testing to gain a clear picture of a patient’s injuries and how they can help reduce their symptoms with the least amount of invasive treatment possible. If you or a loved one have been involved in a car collision, you must ask your medical doctor and chiropractor the difference between a Medial branch Block Vs. and Facet Joint Injection.
As is the case with many spinal injections, facet joint injections are best performed with the assistance of fluoroscopy (live x-ray) to ensure proper needle targeting and placement (and to help avoid nerve injury or another injury).
Facet joint injections and medial branch blocks typically contain two types of medication: a local anesthetic (which relieves pain) and a steroid (which helps to reduce swelling and inflammation). Facet joint injections and medial branch blocks both work similarly but are administered in different locations within the joint. Your doctor will inject a local anesthetic and steroid directly into your facet joint during a facet joint injection. This is done to help alleviate inflammation in the joint space. A medial branch block involves injecting a local anesthetic and steroid directly into the nerves in your facet joint that transmit pain signals to your brain. This will temporarily halt the nerve’s transmission of pain signals.
By numbing the medial branch nerves, a medial branch block can aid in diagnosing whether or not the source of your pain is the facet joints. If the medial branch block alleviates your pain, the source of your pain is more than likely a facet joint.
Medial branch blocks are used to determine whether your pain originates in the facet joints and whether radiofrequency ablation (RFA) may help alleviate your pain. A medial branch block is a procedure in which your pain management specialist uses an anesthetizing drug to briefly stop the medial branch nerves from transmitting pain signals to your brain. If a facet joint problem causes your pain, a medial branch block may provide temporary relief.
If you get significant pain relief through this temporary medial branch block, then you may be a candidate for RFA, which is a longer-lasting interruption of nerve impulses from the medial branch nerves.
What to expect during a lumbar medial branch or Facet Injection block procedure is as follows:
Facet joint injections can be life-changing for millions of people who suffer from lower back pain. Back pain sufferers can experience months of relief with this minimally invasive procedure. The injection may be beneficial if the problem is specific to the facet joints. Otherwise, alternative therapies may be necessary. Consult a physician immediately for an evaluation and treatment of lower back pain. However, as explained throughout this explanation of Medial branch Block Vs Facet Joint Injection, you may have to endure both procedures.
Although most side effects of a medial branch block are uncommon, they do occur. It is common to experience temporary discomfort at the injection site. Certain patients report feelings of weakness or numbness. Occasionally, a minor infection at the injection site develops in a small number of patients. In a much smaller proportion of patients, medial branch block exacerbates pain. If you experience any unusual side effects, contact your doctor immediately.
You may experience decreased pain immediately following the injection. However, this is only a temporary fix until the medication takes effect. This can take between two and seven days following the injection. If the initial injection is effective at controlling your pain, your doctor may perform additional injections. Remember that comparing the results of your Medial branch Block Vs Facet Joint Injection can make all the difference in the world for true, long-lasting pain relief. The amount of relief depends on the nature of your pain, and because the spine contains a variety of pain receptors, the injections’ long-term effects cannot be predicted. Because everyone’s pain is unique, the effectiveness of treatment will vary. The effectiveness of Medial branch Block Vs Facet Joint Injection can also vary, but that is the best way to determine your pain management journey.
Facet joint injections and medial branch blocks have varying success rates. According to studies, up to 92 percent of patients experience pain relief for a brief period of time, typically 1 to 4 weeks after the injection. However, symptoms may or may not recur over time. Certain patients may require additional injections to maintain relief, while others may experience complete resolution or long-term pain relief. In individuals who experience temporary pain relief from facet joint injections, these injections can provide a window of opportunity to progress with physical therapy and other therapies. Strengthening and rehabilitating the neck or back may result in improved function and long-term pain relief. Typically, within a one to four-week period, our pain management specialists must determine which procedure or protocol is the superior choice by comparing Medial Branch Block Vs. Facet Joint Injection.
You can usually resume your normal activities the next day following a facet joint injection. Indeed, some people return to work the following day. There are, however, a few things to keep in mind in the days and weeks following your injection. You should avoid strenuous activity for a few days following the procedure. Instead, gradually increase. It’s prudent to avoid driving for the first 24-48 hours. After the numbing anesthetic wears off, you may experience an increase in pain.
How does your brain determine when you are experiencing pain? How does it distinguish between the gentle touch of a feather and the prick of a needle? And how does that information make its way to your body in time for it to react? How is acute pain transformed into chronic pain? These are not straightforward responses, but with a brief explanation of how the nervous system works, you should be able to grasp the fundamentals.
The nervous system is composed of two major components: the brain and spinal cord, which together comprise the central nervous system; and sensory and motor nerves, which comprise the peripheral nervous system. The names help visualize the concept: the brain and spinal cord serve as hubs, while sensory and motor nerves branch out to provide access to all areas of the body.
Simply put, sensory nerves transmit information about our environment to the brain via the spinal cord. The brain communicates with the motor nerves, which assist us in performing actions. It’s as if you have a highly complex inbox and outbox for everything.
As an example, suppose you step on a rock. How does a sensory nerve in the peripheral nervous system determine that this is not a soft toy? Different sensory nerve fibers respond differently to different stimuli and produce chemical reactions that influence how sensations are interpreted. Certain nerves transmit signals in response to light touch, while others respond to intense pressure.
When there has been an injury, or even a potential injury, such as a break in the skin or a large indentation, specialized pain receptors called nociceptors activate. (Nociceptors are responsible for sending signals to the spinal cord and brain when there is potential damage to the body.)
Even if the rock does not penetrate your skin, the compressed tissues in your foot cause the nociceptors to fire. Now, an impulse is traveling through the nerve and into the spinal cord, eventually reaching the brain. This occurs in a matter of fractions of a second.
Your spinal cord is a complicated network of nerve fiber bundles that transmits a variety of signals to and from the brain at any given time. It functions similarly to a highway for sensory and motor impulses. However, your spinal cord is capable of making some basic decisions on its own. These “decisions” are referred to as reflexes.
The dorsal horn of the spinal cord serves as an information hub, simultaneously transmitting impulses to the brain and returning them down the spinal cord to the area of injury. The brain does not need to communicate to your foot to move away from the rock because the dorsal horn has already done so. If the brain serves as the body’s CEO, the spinal cord serves as middle management.
While the spinal reflex occurs at the dorsal horn, the pain signal is transmitted to the brain. This is because pain is more complex than a simple stimulus-response relationship. Simply removing your foot from the ledge will not resolve all of your issues. Regardless of the severity of the injury, the tissues in your foot must be repaired. Additionally, your brain requires time to process what has occurred. Your brain catalogs pain, and emotions become associated with stepping on that rock.
When a pain signal reaches the brain, it is directed by the thalamus to one of several different areas for interpretation. Several areas of the cortex determine the source of the pain and compare it to other types of pain with which it is familiar. Was it precise? Was the pain greater than stepping on a tack? Have you ever stepped on a rock, and if so, how was the experience? Was it better or worse?
Additionally, signals are sent from the thalamus to the limbic system, the brain’s emotional center. Have you ever wondered why certain types of pain make you cry? The limbic system makes the decision. Each sensation you encounter is accompanied by feelings, and each feeling elicits a response. Your heart rate may accelerate, and you may begin to perspire. All because of a rock beneath your feet.
While it may appear straightforward, the process of pain detection is complicated by the fact that it is a two-way street. It is not even a bidirectional system. Pain is more than a simple cause and effect relationship. It is influenced by the rest of the nervous system’s activity. At any given time, your mood, your prior experiences, and your expectations can all influence how pain is perceived. How’s that for perplexing?
If you step on that rock following a disagreement with your wife, your reaction may be quite different than if you’d just won the lottery. Your feelings about the experience may be tainted if your foot became infected the last time you stepped on a rock. If you’ve previously stepped on a rock and nothing terrible happened, you may recover more quickly. You can see how different emotions and experiences can influence how you react to pain. Indeed, a strong correlation exists between depression and chronic pain.
When Acute Pain Develops Into Chronic Pain
In this case, once your foot has healed, the pain sensations will cease. This is because the nociceptors have lost their ability to detect tissue damage or injury. This is referred to as acute pain. Acute pain does not persist following the healing of the initial injury.
However, occasionally, pain receptors continue to fire. This can be caused by a disease or condition that causes damage on a continuous basis. With arthritis, for example, the joint is constantly in disrepair, resulting in rapid transmission of pain signals to the brain. Occasionally, nociceptors will continue to fire even in the absence of tissue damage. Although there is no longer a physical source of pain, the pain response remains the same. This complicates the diagnosis and treatment of chronic pain.

Facet Injections Vs Manipulation Under Anesthesia
This condition is a deterioration of the Facet joints, which help stabilize the spine and limit excessive motion. The Facet joints are lined with cartilage and are surrounded by a lubricating capsule that enables the vertebrae to bend and twist.
Facet Joint syndrome occurs when the Facet joints become stressed and damaged.
This damage can occur from everyday wear and tear injury to the back or neck or because of degeneration of an intravertebral disc.
The cartilage that covers the stressed Facet joints gradually wears away. The joints become swollen and stiff. The vertebral bones rub directly against each other, which can lead to the growth of bone spurs along the edges of the Facet joint.
Pain from Facet joint syndrome differs depending on which region of the spine is damaged.
If the cervical or upper spine is affected, pain may be felt in the neck, shoulders, and upper or middle back. The person may also experience headaches if the lumbar or lower spine is affected.
Pain may be felt in the lower back buttocks and back of the thigh. For set. Joint syndrome is first treated conservatively with rest, ice, heat, anti-inflammatory medications, and chiropractic therapy.
In addition, Facet joint blocks or injection may be administered not only to diagnose Facet joint pain, but also to treat it.
If nonsurgical methods fail to relieve pain, manipulation under Anesthesia should be performed.
What is the purpose of facet injections?
A facet joint injection may be done to help diagnose the facet joints as the source of the patient’s pain, as well as to provide pain relief. Facet joints are pairs of small joints in between the vertebrae in the back of the spine.
How long do facet injections last?
There is an immediate effect from the local anesthetic which wears off over a few hours. The cortisone starts to work in about 3 to 7 days and it can last up to a few months. Several injections may be necessary over a period of a few weeks to 6 months.
Is facet joint injections painful?
A facet joint injection is a shot of medicine to help with pain from arthritis. The injection goes into your neck or back. … Problems in these joints can cause long-term (chronic) pain in the neck or back. Sometimes the pain is in the shoulders, arms, buttocks, or legs.

Cervical Facet Syndrome
Where is the facet joint located?
Vertebral body, the bony building blocks of the spine. Facet joint, small stabilizing joints located between and behind adjacent vertebrae. Inter vertebral disc, which provides a cushion between each of the vertebral bodies and binds them together.
What Can I expect From A Facet Injection?
After the procedure, the patient typically remains resting in the recovery area for twenty to thirty minutes, and then is asked to perform some movements or activities that would usually provoke their pain.
Patients may or may not obtain pain relief in the first few hours after the injection, depending upon whether or not the joints targeted are the main source of their pain. If the joint or joints being targeted are not causing their pain, a patient will not obtain immediate relief from injection. On occasion, patients may feel numb or have a slightly weak or odd feeling in their neck or back for a few hours after the injection.
How often can you get facet joint injections?
Facet joint injections are generally limited to three within a six-month time frame. In many instances, only one or two injections are required to obtain benefit. Radiofrequency neurotomy or denervation is usually effective after one treatment. Radiofrequency may be repeated every one to two years, if necessary.

Neck Facet Syndrome
Is facet joint pain permanent?
For hundreds of thousands of people who suffer with chronic back pain due to facet arthritis, there is a treatment breakthrough that is completely noninvasive and can bring fast, permanent pain relief. … Inflammation and bone spurs can occur, causing acute pain. Headaches and muscle pain are common complications.
What is the purpose of facet injections?
A facet joint injection may be done to help diagnose the facet joints as the source of the patient’s pain, as well as to provide pain relief. Facet joints are pairs of small joints in between the vertebrae in the back of the spine.
What aggravates facet joint pain?
A car accident, sports injury, or a fall can damage one or more of the facet joints, leading to facet arthropathy. Wear and tear on the facet joints. Heavy lifting, improper posture, and disc problems are some of the factors that can cause the cartilage to wear down.

Facet Syndrome lumbar
Can facet joints cause nerve pain?
Facet joint degeneration can be painless until an event triggers symptoms. … Facet joint symptoms may also mimic the pain of a disc herniation. Pain may be felt down the arms or legs if bone spurs form and press on the spinal nerves.
What medication is used in Facet injections?
A facet joint block or injection is a minimally invasive procedure in which a physician injects a small amount of local anesthetic and/or medication to numb a facet joint and provide pain relief. Fluoroscopy, a form of real-time x-ray, or CT is used to guide the placement of the needle into the facet joint.
Are facet injections safe?
As with all invasive medical procedures, there are potential risks and complications associated with facet joint injections. However, in general, the risk is low, and complications are rare. Potential risks and/or complications that may occur from a facet joint injection include: Allergic reaction.
Can a chiropractor help facet joint pain?
Recent research shows that spinal manipulation of the type chiropractors does and in combination with exercises is the most effective treatment for both acute and chronic facet joint pain. Chiropractors advocate dealing with the underlying neurological, mechanical and muscular problems.
What are symptoms of facet joint problems?
Pain, numbness, and muscle weakness associated with facet joint syndrome will affect different parts of your body depending on which of your nerves are being affected. If the nerves affected are in your cervical spine, you may have symptoms in your neck, shoulders, arms and hands.

Facet Joint Syndrome After Car Accident
Can facet joint cause hip pain?
Facet pain from these joints is quite common. Pain is usually felt directly over the affected joints, but may also be felt in the buttocks, hips, groin, and back of the thighs depending on which facet joint is injured.
Are medial branch blocks the same as facet injections?
A facet block is an injection of local anesthetic and steroid into a joint in the spine. A medial branch block is similar, but the medication is placed outside the joint space near the nerve that supplies the joint called the medial branch (a steroid may or may not be used).
Will facet injections help sciatica?
A facet injection is a minimally invasive treatment option for back pain caused by inflamed facet joints, which may develop from spinal stenosis, sciatica or arthritis, and is characterized by neck, arm, low back or leg pain. … The steroid reduces inflammation and can relieve pain for a few days to a few years.
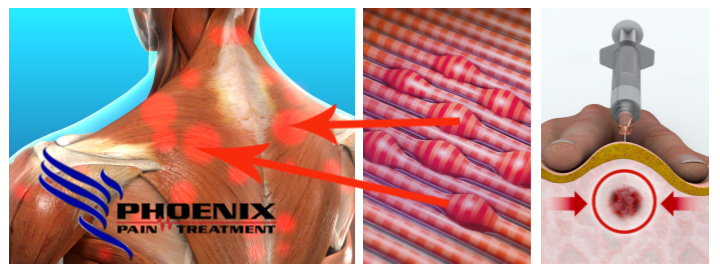
Trigger Point Injections
At Phoenix Pain Treatment our clinicians specifically examine for trigger points which can cause pain and suffering. In this article we hope to shine some light on how actively treating your trigger points will decrease your pain, allowing the affected muscles to relax and help to heal your injuries. A trigger point is a small but highly concentrated muscle spasm which can actually be felt as a small lump or nodule. Pushing on this nodule typically produces pain that can be quite intense. Trigger points can exist in any muscle in your body. More often than not there will be several trigger points in the same muscle or muscles that over lap one another.
Typically following auto accident trauma, especially whiplash injury trigger points can be found on both sides of your body. In the case of whiplash, they can be found in the neck muscles as well as the muscles that connect to the neck from the shoulders. Trigger point cause your muscles to fire and spasm and a muscle that is in spasm is in a weakened state and therefore is not functioning properly. Restricting the muscles range of motion. Trigger point typically cause pain but sometimes are not painful until pressed on. Trigger point pain will refer to different area of your muscles. This is called referred pain and referred pain can make diagnosing and managing trigger points difficult. Referred pain typically follows certain patterns that are well documented. Let’s take a closer look at the trigger point. The trigger points can be palpated by the trained physician, but you have to know what you are looking for in order to find it. That is why we place trigger points in the “Underlying or hidden Injuries” category.
To understand how these seemingly tiny nodules can affect the entire functional capacity of your muscles we have to discuss some anatomy. So think of a muscle as a group of bundles of straws and each straw is wrapped in plastic cling wrap. Then take 2 or 3 or those individual straws and wrap them in plastic wrap. Now do this several times. So each straw is now called a Sarcomere and the plastic wrap is now protecting and connecting the Sarcomeres. Now let’s add blood vessels like arteries and veins and of course your nerves.
So a trigger point would form between the Sarcomere (the straw) and the protective coating (The plastic wrap) which added all together makes up your muscle. In this environment everything is very neatly packaged, and the trigger point causes your anatomy to change and it irritates the Sarcomere and their coverings and causes the nerves to fire giving you pain. When your doctor palpates (or feels) the trigger point immediate referral of pain occurs.
The trigger points cause the micro anatomy of your muscles (Sarcomeres) to stay in a spastic state giving off pain signals to your brain and your brain in turn tells the muscle to shut down. It is really a cascade of decreased oxygen, nutrient starvation and waste product builds up because everything is just not functioning correctly. It gets even worse as the trigger point continues your muscle actually shorten and can become even tighter and more painful. More often than not trigger points will not just go away on their own.
The first line of management of trigger points is to massage the trigger points in order to help them release. This can be very painful for the accident victim to endure. The idea is to massage the trigger point area to increase blood flow and with that comes increased oxygen and nutrition and hopefully getting the waste products to move out of the area.
When this does not occur our Chiropractic physicians will refer out for Trigger Point injections. The idea is to get the trigger point to release and sometimes this takes a concerted effort for both chiropractic and interventional pain management to get the trigger points to release. So the interventional pain medical doctor injects the trigger point with anti-inflammatory and pain relieving medications. Don’t worry injection uses a very tiny needle and is not very painful at all. There is typically immediate decrease of pain and tightness. You would then go back to your conservative physical medicine delivered by your chiropractor. Trigger points will require 1-2 injections.
If you or a loved one have been involved in an auto accident it is likely that you may have trigger points in the muscles surrounding the affected area. Give us a call today.

Call Now Phoenix Pain Treatment 602-449-9430
Phoenix Pain Treatment provides phoenix pain treatment that combines international pain management, phoenix chiropractic treatment and alternative non-pharmacological alternatives to long term oral medication. Premier Pain Solution combines the best of Medicine and alternative treatment such as Scottsdale pain treatment and manipulation under anesthesia to achieve a viable solution for your pain relief with lasting results.
Here are a few resources for you concerning drug less non-pharmacological or non medication alternatives for the pain you may be suffering with.
http://www.advancedsportschiropractic.comWed, 17 Apr 2013 21:19:00 GMT
asc_small_simple_logo. A slipped disc is the common term for a prolapsed or herniated spinal disc. These discs are set in position between the vertebrae and do not “slip”. Instead, the disc’s outer, fibrous ring tears, there …
[iframe width=””][/iframe]
http://www.wikipedia.org/wiki/Spinal disc herniation
A Spinal disc herniation (prolapsus disci intervertebralis) is a medical condition … the condition include herniated disc, prolapsed disc, …
Injuries sustained in automobile and motorcycle accidents make up one of the most common causes of chronic pain. Thousands and thousands of people are injured in motor vehicle accidents every day in the U.S., but many of these injuries are not readily apparent.
Even when a car accident seems like it’s not very serious in terms of damage to the vehicles involved and outward signs of physical trauma to their occupants, hidden injuries can bring on serious, long-lasting pain that may significantly reduce the sufferers’ quality of life and that may interfere with their ability to work and enjoy life as they wish.
If you’re involved in a car accident, paramedics on the scene will check first and foremost for life-threatening injuries. If you are taken to the emergency room, the emphasis again will be on detecting any acute problems that must be addressed before you can be sent home. Injuries like broken bones and bleeding lacerations are relatively easy to detect, but the injuries that cause chronic pain are not so obvious. To make matters more confusing, the pain itself might not be felt for some time after the incident that triggered it.
In fact, the onset of serious pain most commonly does not occur until three days after the incident that caused it, and it can take even longer than that for chronic pain to become evident. In an accident, the vehicles involved often experience near-instantaneous deceleration; that is the cars or trucks are quickly brought to a stop when they collide. The problem is that the human bodies inside, following the laws of physics, continue traveling in the same speed and direction that they were already going.
Fortunately, the vehicles’ restraint systems keep them from doing so, otherwise many accident victims would fly through the windshield and land on the pavement, as used to happen more often in the days before widespread use of seat belts. Unfortunately, the forces applied by the sudden stoppage can wrench a human body violently enough to cause trauma to the soft tissues around the joints, that is, the muscles, tendons and ligaments around areas such as the knees, shoulders, elbows and hips. The neck is one of the areas most prone to injury in a car accident; injuries that happen to the tissues around the upper spine are often collectively referred to by the non-medical term whiplash.
Phoenix Pain Treatment offers Phoenix interventional pain management for auto accident victims. Not only do we offer many modalities of medical and chiropractic treatment for pain, we can help you navigate through the complex and often difficult legal and insurance issues that often surround getting treatment for an accident-related injury. If you have post-accident pain, call Phoenix Pain Treatment at 602-449-9430.
Fibromyalgia, if left undiagnosed and untreated, can make its victims’ lives miserable. Fibromyalgia causes those suffering from it to experience chronic widespread pain and sensitivity to pressure, sometimes along with numbness and tingling sensations. Fibromyalgia sufferers usually also experience stiffness of the joints, disturbed sleep and chronic fatigue.
While fibromyalgia is not a degenerative or progressive disorder and does not lead to death, it’s a very difficult condition to deal with. In fact, the emotional toll of living with fibromyalgia may have as great an effect on a victim’s quality of life as the actual physical symptoms. Fibromyalgia appears to impair some victims’ ability to think, as well. The combination of physical pain, cognitive impairment and mood effects such as depression and anxiety causes many fibromyalgia sufferers to change jobs, cut back their work hours or quit working altogether, often creating a severe financial strain that affects their quality of life even more.
Fibromyalgia affects an estimated 2 to 6 percent of the world’s population; in the United States, there are an estimated 10 million fibromyalgia sufferers. The great majority of fibromyalgia victims are women. According to the National Fibromyalgia Association (NFA), 75 to 90 percent of people diagnosed with fibromyalgia are female. In women, the diagnosis of fibromyalgia (sometimes abbreviated FM or FMS for “fibromyalgia syndrome”) usually occurs during the childbearing years.
Despite the preponderance of cases among women aged 20 to 50, fibromyalgia can and does strike people of both genders and of all ages and races. The prevalence of FM does go up among the elderly, however – the NFA says that by age 80, about 8 percent of the population meets the criteria for a diagnosis of fibromyalgia established by the American College of Rheumatology.
Although the syndrome has probably been around for most of human history, the term “fibromyalgia” was not coined until 1981. The word is a combination of Latin and Greek words meaning “connective tissue and muscle pain.” In the past, the symptoms of fibromyalgia may have been labeled “muscular rheumatism” or “neurasthenia.”
Doctors and researchers do not agree on the causes of fibromyalgia. A predisposition to fibromyalgia might be passed on genetically, but stress in one’s environment seems to be a contributing factor, too. Fibromyalgia is also strongly associated with depression. The most accepted hypothesis seems to be that fibromyalgia is caused by a chemical, electrical or physical abnormality (or some combination of the three) in the central nervous system (CNS). A victim’s pain threshold is lowered because the CNS responds with greatly increased sensitivity to everyday movements and pressures that would not cause pain in a healthy individual. Just because fibromyalgia may originate in the nervous system, however, does not mean that it’s a mental disorder. Often victims are told “it’s all in your head,” which only makes the situation more difficult for the fibromyalgia sufferer.
No single test exists for fibromyalgia, but the American College of Rheumatology established criteria for diagnosing fibromyalgia two decades ago. To be diagnosed with fibromyalgia, a patient must have a history of chronic widespread pain that has lasted at least three months and that affects all four quadrants of the body — upper left, lower left, upper right and lower right. Also, a person must feel pain when pressure is applied to at least 11 of 18 designated “tender points” located in various areas of the body. These possible tender points occur in pairs on the front and back of the neck, shoulders, elbows and knees as well as on the lower back and just below the buttocks. It should also be noted that a fibromyalgia sufferer is likely to feel pain in other areas besides these tender points.
The healthcare providers at Phoenix Pain Treatment offer Manipulation under Anesthesia (MUA), which breaks up the affected fibrous tissues of the muscle and ligaments, allowing you much more freedom of movement. This in turn also allows the nerves within the muscle tissues to have a more natural relationship, so that the nervous tissues are able to relax and not be as irritated by the fibrous tissues inherent with fibromyalgia. If you’re suffering from fibromyalgia pain, call the caring staff at Phoenix Pain Treatment at 602-449-9430.